Saturday, March 24, 2012
Re-Defining the Joint: Part 3
It has been quite awhile since the posting of part 1 and part 2, however there has been a recent ¨spike¨ in reads for both parts (currently rank #2 and #9 in the top 10 reads) therefore I think it is an appropriate time to complete the trilogy. As per part 1 and 2, a radical alteration of conceptual understanding of joints must take place in order to fully grasp (and appreciate) the complexity of human movement.
I read a book called The Structure of Scientific Revolutions that effectively demonstrates a ¨fatal¨ flaw in the evolution of science...most (if not all) of the new ¨scientific discoveries¨ are derived from already established paradigms. To be specific, research into human movement and (bio)mechanics assumes that the traditional mathematical model (single pivotal movement) is the ¨law¨...therefore every hypothesis, design, conclusion is derived from this ¨fact¨. Common sense dictates that, if the overriding paradigm is flawed (or otherwise over-simplified), then the results / conclusions will also be so. Although over-simplification has some merit in making treatment protocols easier to ¨digest¨and conform to current health care delivery methods, it does not mean than more precise and effective understanding should be ignored. In fact, deeper understanding does not disregard the current formula...rather it ABSORBS IT.
In order to fully appreciate part 3, I suggest a read (or re-read) of parts 1 and 2. However, to summarize the main message:
The true definition of a joint must be expanded into a broader understanding that it is the linear or angular displacement between separate biological elements. Therefore, simple pivotal movement is only a fraction of the equation. There are 2 fundamental realities that also exist alongside of the classical mathematical model:
1) Fascial Articulations: This term defines the very real movement potential between the individual fascial layers that exist from the surface of the skin to the periosteum of the bone (and indeed even deeper into the very cell itself).
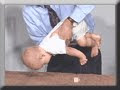
The above image illustrates an example of the fascial relationship between muscle/tendon and adjacent structures. Effective movement requires, not only proper ¨connective¨ elements, but selective ¨DISCONNECTIVE¨ properties. In other words, the ¨sliding¨ (hence articulation) of fascial layers between each other is essential. By definition, this constitutes a joint...without these characteristics, movement potential is significantly altered leading to movement dysfunction, irregualr load bearing and stress distribution, and ultimately deterioration.
2) Movement is more precisely ¨Gear-like¨: This is perhaps confusing and counter-intuitive, however it is none-the-less a reality. The pivotal model suggests that movement is a summation of single pivots moving at the same time. Once again, this is a serious over-simplification.
True function is achieved through a complex of gear-like movements that are NOT the sum of individual movements rather a single unified systemic response.
The image to the left clearly illustrates that single pivotal movement (hip joint) is effectively a small contributor to the performance of a straight leg raise (hip flexion). This movement is defined by gear-like movement between the individual vertebrae of the lumbar spine, the pelvis, and the hip. In addition, this requires proper fascial articulation (sliding) of the fascial layers of the posterior leg.
It is precisely these realities that highlight some of the current flaws in assessment and evaluation protocols. The fundamental question remmains: how can an effective treatment protocol be formulated when only one third of the mechanism is observed and identified??! At best, these types of approaches will be successful only 33% of the time and/or resolve only 33% of the initial problem. The concept of re-defining the definition of a joint only serves to enhance understanding and by default result in more effective interventions.
The switch from pivotal understanding to the ¨gear ratio¨ perspective will provide some valuable insight and clarity into the amazing movement potential of the human body. I am reminded of an ¨Old School¨ kids game called Spirograph. My brother and I played with this quite alot, but it has its merits from a conceptual perspective.
It involved placing variuos small gear-like tools into the center of a larger circle with gear teeth. You would then insert pencils of different colour into the smaller gear and spin it around the outer circle. The result was a myriad of amazing shapes and images.
Although it is a simplistic analogy, it reveals the sophistication and complexity that exists in this model...whch is reflected in the everyday marvel of human movement.
I hope this trilogy has been both informative and insightful. If nothing else, it serves as an example of the need to reach beyond current accepted paradigms in an effort to evolve your understanding.
Cheers.
Saturday, March 17, 2012
The Student Becomes The Teacher
Every once in awhile it is good to stop and engage in some serious introspection. I mean this from a purely professional perspective. To be precise, the designation of ¨professional¨ assumes some level of competency that is superior to that of those who seek your help. On some levels this is true...however, the harsh reality is that many take this too seriously. I truly believe that true professionalism is the CONTINUING search for more understanding as well as being conscious of the fact that there is so much more yet to learn.
It is in this light from which the inspiration for this short post was formulated. I am once again working with the ever-enthusiastic ABR (Advanced Biomechanical Rehabilitation) families from Rosario, Argentina and I experienced a very encouraging event. My role with these families is, at it´s essence, that of a coach or mentor...however this time I was pleasantly surprised to be the student for a short time! For those who are unfamiliar with ABR, it is a very innovative technique that is taught to the parents of children with Cerebral Palsy (and other disorders of movement and posture) so that they are able to deliver consistent and comprehensive treatment directly in the home. There are a multitude of applications and guidelines that require regular skill development for which I am responsible for providing.
Each individual child is unique in their priorities, manifestations, and challenges...which makes the implementation of each application unique in itself. On some occasions, particular applications can be challenging and can sometimes present some difficulties to us ¨coaches¨. I was therefore very encouraged when I saw a father (Ivan Cief...a naturally skilled ABR provider) performing his own version of a particular application. This inspiration came from intelligent and analytical thinking on how to best deliver a specific technique (Submerged Shoulder) given the unique characteristics of his daughter.
It is then that I put on my ¨student´s hat¨ and grabbed my camera. Ivan´s carefully formulated adjustment opened the door to some very interesting and new possibilities for positioning that will hopefully be translated into future improvements and evolution of the technique. I will be (unofficially) calling this the ¨Uma Position¨...which will be a continuing reminder that some cliche´s (however much we hate to hear them) are true: the best teachers learn from their students!
Hats off to Ivan and Team Uma!
Monday, February 27, 2012
The Fibroblast
Another brief rant on the fundamentals of understanding the role of fascia and connective tissue. Although there are many specific topics to uncover, there isnt a better place to start than getting familiar with the Fibroblast.
A fibroblast is a cell that essentially produces and maintains the Extracellular Matrix of the connective tissue...or to put it simply, the ¨caretakers¨ of the connective tissue. It does this by secreting precursors into the extracellular matrix which maintain the structural integrity of the entire system.
The most important characteristic to remember about the Fibroblast is that it is adaptive. They provide the architectural plan for the fascial system and therefore react and adapt to tensional / compressional (Tensegral) stress. Through Mechanotransduction (see previous post: Mechanotransduction), it can transmit forces within the cell as well as from cell to cell through tensional forces. Why is this so important? Fibroblasts provide the architectural framework for bones, nerves, blood, fascia, etc...and therefore all of the structures that depend on those structures.
It is important to remember that the specific adaptation exhibited by the fibroblast is dependant on the mechanical force applied...therefore rendering the type of intervention (also the mode of intervention) a critical consideration for the care-seeker.
In most disorders of movement and posture (Cerebral Palsy, etc) and even most chronic pain disorders, there is a significant weakness / dysfunction of the connective tissue system. This is manifest a a pure weakness of the tissue itself or in a symptomatic way (muscular tension as a result of connective tissue fatigue or failure).
In summary, understanding the fundamental ¨building blocks¨ provides valuable insight into the development, management, and maintenance of the megstructure.
Cheers!
Tuesday, February 14, 2012
The ¨SuperTendon¨ Concept
Once again, I have been bitten by the ¨nerd bug¨and have been plowing through some of the scientific articles that are continually piling up...with no end in sight. I consider this both a blessing and a curse: although it is obvious that I do not possess enough years in my lifetime to absorb everything, each new read sheds even more light and understanding.
I have recently been examining the ¨Form and Function¨relationship...more specifically, the concept that form (structure) IS function. With this in mind, I came to focus on a particular article that had previously gone unnoticed. Upon reading through it, I was pleasantly surprised to finally find a ¨user-friendly¨ article that captures the essence of the Transanatomical understanding of human form and function. To be precise, it exposes the limits of the popular Topographical Anatomy understanding when it comes to analyzing function...which therefore renders any rehabilitative strategy to something relatively simplistic.
It is through works like this...as well as the mentioned Frederic Wood Jones and Buckminster Fuller...that we get a more comprehensive understanding of the intimate relationship between the ¨Bioengineering¨of the human organism (form) and our interaction with the environment (function). More to come on the works of Wood Jones and Fuller, but this article should provide an effective entry into the transanatomical mindset.
Structure-Function Relationships in Tendons
Thursday, February 9, 2012
Success in the Fascial Paradigm: Passive-Aggressive Therapy?
I have chosen this photo to lead off this post for a very straightforward reason: it is time for the "therapeutic world" to take off the noise-cancelling headphones and start to acknowledge the undeniable potential of the fascial paradigm in the treatment of Cerebral Palsy and other disorders of movement and posture.
I think it is EXTREMELY important to also acknowledge the generous and unselfish contribution of Nancy and Haroldo Guerrero who have given me permission to use the images of their child to further contribute to the overall good and education of families and professionals alike. It has been my honour and pleasure to have been able to work with them for the last 4 years...and I am humbled by their dedication, work ethic, and superior frame of mind. Therefore on behalf of myself and all of the readers of this post...GRACIAS, NANCY Y HAROLDO!
Although a comprehensive history is always recommended, I will abbreviate this particular history in an effort to remain within a "digestible" amount of information. Matias is a severely affected child who obviously manifests a great deal of musculoskeletal challenges. This manifestation is most easily observed as muscular tension, rigidity, and stiffness. Within the traditional musculoskeletal paradigm, this tension is considered the "problem" therefore it is given primary focus and is the target of selective intervention (stretching, Botox, surgery, tenotomy, etc). As mentioned before in this blog (see previous post "Spastic Muscles: Victim or Perpetrator"), the muscles are SYMPTOMATIC. Therefore, they REFLECT an underlying problem and are therefore considered victims. By definiton, it is unproductive to set them as the primary rehabilitative focus. The true "perpetrator" is the lack of compressional strength (postural strength) which is mediated by the fascial system. There will be a large number of people / professionals scratching their head at this statement..."that doesn't make any sense whatsoever". With all due respect to them, my simple reply would be that it doesnt make sense to them because that's not what they read in their textbooks! My best advice would be to close those books...look at things more analytically...and formulate your own conclusions. This in itself is a difficult task...therefore I propose a simpler approach which comes in the form of a simple fundamental question that you should ask yourself: IS IT POSSIBLE TO IMPROVE THE STRUCTURE OF A SEVERELY AFFECTED CP CHILD WITHOUT ATTACKING THE MUSCLES THEMSELVES? As you should have already guessed...my answer is a resounding YES!
This simple fact leaves no denying that a more passive, less invasive / aggressive should always be considered first. I admit that simple words are rarely enough, so I am very happy to share some very positive results on what can be generally considered a difficult case.
For those who are not familiar with the Scribd program I use for posting documents: You must click the title (in blue) of the document to download it. You will likely be able to read it directly from my blog, just use the scroll bar on the right hand side. It may be small lettering for some...so please be sure to click and have a look directly on Scribd if necessary!
Success in the Fascial Paradigm
Thursday, February 2, 2012
Mechanotransduction: Response to Manual Therapy
For the very few regular readers, I must apologize for the long delay between posts. My unofficial rule is to produce 3 or 4 posts per month...however it seems that newborn babies do not follow this rule! Now that I have had a few months to adjust, recharge, and refocus, I will begin my "re-entry" into the blogosphere with a short back to basics post.
I have recently been clicking through the Inger Lab web publications (a very good site for those fascia nerds like me) and I came to the realization that a great deal of information is right under our noses...it just requires some effort in "digging" for it. What do I mean by this? Most people have the obvious and instinctive understanding that "if I go to get manual therapy, I will feel better". For most, this basic understanding is sufficient...for example, I need not know HOW a touchpad on a computer works. I need only know that that it does indeed work. But for the more investigative mind (both care-giver and care-seeker), the question still remains "how does the active manipulation of tissue translate into an immediate (or long-term) response? The answer is MECHANOTRANSDUCTION. To put it simply, Mechanotransduction is the process by which cells (and therefore tissue itself) sense mechanical stress and convert these stresses into biochemical signals. On a cellular level, the signal is sent to the nucleus and thus affecting the tissue on a "macro" level by promoting healthy remodelling.
As the above image so elegantly illustrates, the cell itself is a Tensegral construction that intimately connects the entire organism. Depending on the type of stress (sheer, compression, tension, etc), the cell will respond differently. Therefore, the TYPE of manual application is vitally important as well as the MODE of delivery (light, aggressive, quick, slow, etc).
With respect to the Fascial Paradigm, this is a key understanding and fundamental principle. Remodelling of connective tissue is always the ultimate goal, however the promotion of HEALTHY remodelling is the key.
My parting message is simple: Even the smallest biological element (cell) can sense differences in mechanical stress. Therefore the focus on the characteristics of the application of the manual therapy technique become more than important...they are critical! Mechanotransduction shows us that there is true power in the effectiveness of manual therapy...the real "skill" comes with the understanding of the specific mechanisms of application and response.
Thanks for reading!
Sunday, November 20, 2011
Cerebral Palsy and the Pediatric Evaluation
Part 2: The Developmental Process: Primitive and Postural Reactions
The second installment in this series on Understanding the Pediatric Evaluation revolves around two fundamental elements of the developmental process that are critical in the greater understanding of the long-term rehabilitation plan. Primitive and postural reactions are characteristic of critical early development that effectively signal progression and movement towards improved development. They are the easiest, earliest, and more frequently used tools in assessing neurological and motor development in newborns and infants.
Primitve Reactions
Primitive reactions are mediated in the brainstem and are fully present at birth. They are characterized by automatic movement patterns that become more difficult to elicit after the first 4-6 months of life. Some examples below:
Moro Reaction: The Moro reaction is obtained by holding the baby’s head and shoulders off of the mat with the arms held in flexion on the chest. The examiner suddenly lets the head and shoulders drop back a few inches while releasing the arms. The arms should fully abduct and extend, then return towards the midline with the hand open and the thumb and the index finger forming a “C” shape. An absent or incomplete Moro is seen in upper motor neuron lesions.
Prone: In the prone position, the baby should be able to extend the neck to the point where the head can be turned side to side. When the arms are extended by the side of the trunk, the baby should be able to bring them forward into a flexed position. The buttock should be somewhat elevated because the hips are flexed and adducted. A baby that is flat on the mat and can’t turn the head back and forth has low tone and weakness.
Head Lag: Starting in the supine position, the baby is pulled by the arms to the sitting position. The head and the arms are observed during the maneuver. The arms should remain partially flexed at the elbow and the head may lag behind the trunk, but should not be fully flexed backwards. When the baby is in the sitting position, the head should be able to come to the upright position for at least a few seconds before dropping forward or backward.
Postural Reactions
Postural Reactions develop following / during the disappearance of the primitive reactions. They can be considered voluntary actions that are produced by multiple sensory and structural inputs. They are complex motor responses to afferents like tendons, joints, skin, internal organs, and even the eyes and ears. They are characterized by predictable postural adjustments to specific applied sudden changes in position. As the child develops, the postural reactions (or postural performance) improve and manifest in more comprehensive ways as he /she ages. Some examples below:
Head and Trunk Control: When pulled to a sitting position, a baby this age should be able to have only slight head lag and, when sitting, the head should be upright but there may still be some wobbling of the head. The back is still rounded, so the baby slumps forward.
Prone: In the prone position, the baby is now able to bring his head up and look forward with the head being 45 to 90 degrees off the mat. Weight is borne on the forearms. When the head and chest are well off the mat, the baby is ready to start to roll from the prone to the supine position. Rolling front to back usually occurs at 3 to 5 months of age. Rolling over too early can be due to excessive extensor tone.
Lateral Propping: Lateral propping or protective extension is essential for the baby to be able to sit independently. This postural reaction develops at 5 to 7 months of age. Anterior propping actually develops first, then lateral propping. For anterior propping the baby will extend the arms forward to catch himself and prevent falling forward. Lateral propping occurs when the baby is falling to one side or the other and he extends the arm laterally to catch himself.
The understanding of these reactions is fundamental in the effective and accurate assessment of the success of the rehabilitation protocol. To be more precise, Infants with cerebral palsy have been known to manifest persistence or delay in the disappearance of primitive reflexes and pathologic or absent postural reactions. Therefore, the emergence of postural reactions (and the reduction of primitive reactions) is the primary treatment goal and thus any protocol that promotes this will ultimately contribute to improved function.
Part 1 of this series identified the need to place primary focus on the developmental age rather than the chronological age. Although not age appropriate, the persistent appearance of primitive reactions in older children is simply an indication of their current status and placement along the developmental path. It should also be remembered that the actual "manifestation" of these primitive reactions may look significantly different in an older child than a 6 month old. The structural proportions (length, weight, mechanics, torque, etc) are very different, therefore the same "reaction" may subjectively appear to be more severe or, at times, appear to be something completely different.
What does this all mean and how does it apply to my understanding of Cerebral Palsy? The answer is quite simple and straight-forward: the developmental process is something that cannot be circumvented or skipped. If the child with Cerebral Palsy continues to manifest primitive reactions in conjunction with the absence of postural reactions,any expectations of higher order function (crawling, independant sitting, gross / fine motor skills) is unrealistic. Rather than a message of "gloomy reality", the fundamentals of the development of the human organism will allow you to understand the "right path" and therefore effectively reduce any unecessary anxiety and worry associated with the unknown. More importantly, it clearly identifies those interventions that are essentially "shortcuts" along the path...which initially produce increased levels of hope and expectation, but in the end reduce maximum potential.
I apologize for the relatively longer post...it has been quite the challenge to even keep it this short! The third installement: Cerebral Palsy and the Pediatric Evaluation: A Case Study Report will blend the theoretical elements of part 1 and 2 and demonstrate their application in a practical examination of the progress of an actual CP child. I hope that it achieves my goal of creating a link and close the loop of understanding.
Saturday, November 12, 2011
Success story in progress
I am pleased to share a post from one of my ABR families who just recently finished a training session a couple of weeks ago here in Rosario, Argentina. Over the last couple of years, I have had the pleasure and honour to participate in Salvi's evaluations...and at each step he demonstrates continued progress and improvement. I recommend that everyone have a look at this post...but further to that, take time to browse the blog itself. The insight into a family's challenges and successes will be invaluable to anyone. Click the blue link below and enjoy. Cheers!
Creciendo con Salvi: Evaluación ABR noviembre 2011: Es muy difícil para mí intentar resumir todo lo que se habló en la última evaluación de Salvador. Fue muy intensa para mí, con muchísimo fun...
Saturday, November 5, 2011
Cerebral Palsy: Understanding the Pediatric Evaluation
Part 1: Fundamentals in Perspective
I thought it would be a good idea to begin this series of posts with a certain aspect that, in my opinion, is typically missing from most people when entering into any form of evaluation or assessment. It is not my intention to pass judgement on parents, professionals, or any other group of people...it simply exists. What is the missing ingredient? Perspective. Quite simply, the expectations of every parent with a child with CP must be tempered by the proper perspective. Without it, expectations can often run wild and ultimately lead to dashed hopes and unecessary feelings of guilt, frustration, and desperation.
Therefore, the question becomes: "What is the proper perspective?". The answer has been right in front of our (parents and professionals alike) noses. Conditions such as Cerebral Palsy, West Syndrome, etc...fall under the umbrella of Developmental Delay. Simply put, there is a significant delay in the development of healthy motor function. This is a reality that is inescapable...as chronological age proceeds at a regular pace, the developmental process lags behind. Therefore, by definition, the progression of each developmental phase is the ONLY component that matters when gauging progress. It is essential to remember that EVERYONE must pass through these developmental stages...irrespective of their chronological age. The very definition speaks for itself: Developmental Delay (CP) is characterized by the persistence or delay in the disappearance of
primitive reactions and pathologic or absent postural reactions. The vast majority of parents are focused in on the chronological age of their child and therefore attribute "age appropriate" expectations for their child. As mentioned in one of my previous posts: focused attention to your child's developmental age will give you the proper perspective on how they are "hardwired" to develop and therefore foster realistic expectations going into each evaluation or assessment.
Hopefully this small introduction serves to facilitate efficient absorption of the elements in Part 2 (The Developmental Process: Primitive and Postural Reactions).
Cheers!
Saturday, October 22, 2011
Pediatric Evaluation 101
I typically avoid back-to-back posts...prefering to let a post "marinate" in the minds of the reader for at least a week. However, I have recently been actively involved with my work with children with Cerebral Palsy (ABR) and it has only recently occured to me that alot of our evaluation protocol is still somewhat foreign to the many parents and family members. The purpose has become so integrated in my mind, that I haven't truly considered that anyone wouldn't understand, not only WHAT I'm doing, but WHY I'm doing it. In essense, I have overlooked an essential element of any successful assessment: UNDERSTANDING BY THE PARENT / CARE-SEEKER.
With this in mind, I have decided to post a series of "back to school" postings designed specifically to EDUCATE parents on the essentials of typical pediatric assessment protocols. It is my firm belief that, with understanding, you will become more involved in the process of your child's development. In this spirit, I have used a photo of Concordia University in Montreal at the beginning of this post. Not only did I receive my Bachelor of Science degree there, but I went on to teach as a laboratory instructor for 5 fun-filled years. So....class, attention please:
The first "class" is simply to familiarize you with a few basic tests and give you some insight into its purpose. Before I continue, I will remind you of an important point I raised in a posting from June (Trainers Corner: Back to Basics): Consider your child's developmental age in light of the chronological age. In children with disorders of movement and posture, improvement is gauged by the progressive movement through developmental milestones. Therefore, the normal developmental process is your guide. The following are some select tests, with their respective rationale and corresponding developmental stages:
The Prone Position: In the prone position, the baby is now able to bring his head up and look forward with the head being 45 to 90 degrees off the mat. Weight is borne on the forearms. When the head and chest are well off the mat, the baby is ready to start to roll from the prone to the supine position. Rolling front to back usually occurs at 3 to 5 months of age. Rolling over too early can be due to excessive extensor tone. In essense, any functional performance that includes rolling or propping on the hands is dependant on this prior stage.
The Landau Reflex: The Landau is an important postural reflex and should develop by 4 to 5 months of age. When the infant is suspended by the examiner’s hand in the prone position, the head will extend above the plane of the trunk. The trunk is straight and the legs are extended so the baby is opposing gravity. When the examiner pushes the head into flexion, the legs drop into flexion. When the head is released, the head and legs will return to the extended position. The development of postural reflexes is essential for independent sitting and walking. This particular test is not typically done, but can be valuable when more comprehensive discussion on sitting and walking become realistic.
Lateral Propping: Lateral propping or protective extension is essential for the baby to be able to sit independently. This postural reflex develops at 5 to 7 months of age. Anterior propping actually develops first, then lateral propping. For anterior propping the baby will extend the arms forward to catch himself and prevent falling forward. Lateral propping occurs when the baby is falling to one side or the other and he extends the arm laterally to catch himself. Asymmetric lateral propping can be an early sign of hemiparesis. The baby will prop on one side but on the paretic side he will not extend the arm to catch himself.
The Parachute Test (Flying Test): The parachute reflex is the last of the postural reflexes to develop. It usually appears at 8 to 9 months of age. When the baby is turned face down towards the mat, the arms will extend as if the baby is trying to catch himself. Prior to developing this reflex, the baby will actually bring the arms back to the plane of the body and away from the mat.
Traction Test: On traction, which is pulling to a sitting position, the baby has good head and trunk control. The head and shoulders are flexed forward and the arms are flexed. The baby actively helps himself to get to the sitting position by pulling with the arms. Also notice that the legs are flexed at the hips and are off the mat as the baby pulls himself to sitting. On being laid back down to the supine position, the baby doesn’t flop back, but is able to control the lowering of his head and trunk to the mat. This particular test should be very familiar to the ABR readers. How is "good head control" assessed? More importantly, what are the bare essentials needed to have minimal head control? The traction test is a valuable tool that gives excellent feedback and lends towards a more efficient treatment protocol.
In North America, coffee is just as important to the learning process as is a laptop...so, grab a cup of "Joe" (for my South American friends, un cafe con leche) and get to work.
Class dismissed.
Cheers! =)
Friday, October 21, 2011
The Anatomy of Function
This post is intended "for all audiences", however I have formulated it with all of my ABR families in mind. I hope that it sheds some light on a bigger picture...which is sometimes lost in the daily challenges of life.
I think the title gives this post an appropriate "flavour"...thats is to say, we are going to DISSECT function. To be more accurate, it is more of a "de-construction". Function (or better function) is, to say the least, the ultimate goal of any care seeker...and most certainly all of you ABR parents. Therefore, function is an "end"...or a destination. By definition, a destination (or end) must have a starting point and a middle. To be precise, the goal is DEFINED by the journey! Therefore FUNCTION is the sum of component parts. What are the component parts, you ask? STRUCTURE, STRUCTURE, STRUCTURE. You do not have function without structure.
We see this everyday...on every street corner...and in every aspect of our life, but yet it seems to elude us when we get into issues of the human organism. A simple stopwatch from the 1950's (see above image) is an excellent example. A simple function (telling the time) is dependant on hundreds or thousands of smaller structural components working together. For you ABR folks...remember this watch! Functional performance DEPENDS on each piece being in the right place! How would this watch perform if even one of its component pieces were slightly out of alignment? Of course, the human body is not a stop watch...it is exponentially more complex. This truth is precisely the point...if this applies to a "simple" mechanism, then it applies to more complex mechanisms as well.
Even down to the microscopic level, cells are structurally arranged in such a way to, not only function systemically, but to sense mechanical forces and convert them into biochemical changes. This phenomenon is called mechanotransduction. Therefore there is a hierarchy that starts at the smallest level (cells) and extends to the macrostructures (tissues, organs, etc) to reveal a fundamental reality: Structure and Function are seemlessly integrated. You cannot disentangle them...they are intimately related. Structure is the language of function.
So...attention all ABR families curious enough to read this far: Remember this intimate relationship and store it in your mental hard drive. This is precisely the reason we focus so intently on the shoulder blade...the clavicles...the circumference of the thorax, for example. These structural components are the "architectural" foundations of the performance of the arm!
Consider the tired watchmaker peering through the magnifying glass and putting each tiny spring and each tiny geer wheel in place. As each component is put in place, he is that much closer to a functional timepiece!
Saturday, October 15, 2011
Re-defining The Joint: Part 2
This post is intended to supplement my earlier post "Re-defining The Joint: Part" and to continue the journey down the trans-anatomical road of discovery (or re-discovery, to be precise). If you haven't read part 1, I would recommend that you refer to that post before moving on with this one. It will certainly help in the understanding as well as give valuable insight as to what the main message is.
http://thescienceofphysicalrehabilitation.blogspot.com/2011/09/redefining-joint-part-1.html
To briefly summarize, I have proposed a revised definition of a "joint" as: Linear and/or angular displacement between separate biological elements . This definition is more precise and accurate...but it also opens up an entirely new perspective on what actually constitutes a joint. As previously mentioned in my blog, connective tissue has 2 appearances which are seemingly paradoxical: it connects AND disconnects! The connection element is the obvious one (tendons, ligaments, joint capsules, etc) whereas the "disconnection" function is somewhat more counter-intuitive. If you haven't seen Gil Hedley's Integral Anatomy Series videos, then I highly recommend you make a point to watch them. Using standard dissection methods, he intelligently demonstrates the fundamental role of fascia (connective tissue) in SEPARATING body compartments, muscular groups, and systemic organs so that they do not mechanically influence each other. In essense, it allows the elements to "slide" against each other. For example, the liver "articulating" with the diaphragm, deep muscles of the hand (flexor digitorum profundus, for example) sliding underneath the more superficial muscles in the forearm when the fingers are flexed. It doesn't matter whether we actually agree on the definition of a joint...the reality is that without this fundamental characteristic, we would not be able to move...period. We would be as mobile and functional as a Ken (or Barbie) doll..."watered down" to simple hinge joints mixed with a couple of ball and socket joints for good measure.
Therefore, we must add to the understanding and definition of what a joint truly is. This will require some additional qualifying of the term "joint" when making statements or comments. We can consider our typical understanding of joints as SKELETAL ARTICULATIONS...because that's what they are. Therefore, I bring in a new term: FASCIAL ARTICULATIONS.
Each separate colour represents an individual fascial "compartment" and therefore can be considered as a separate biological element. This concept is easily extrapolated into the extremities as well...each individual muscle, muscle group, etc. is compartmentalized as well. It is important to remember that, when we are active (moving), these elements are articulating between each other! Consider a typical tennis swing...with its significant rotational components within the spine. There is a considerable angular displacement between the endothoracic fascia (fascia of the thorax) and the extended fascia of the abdomen (peritoneum). In addition, the follow-through of the arm at the completion of the swing is achievable through, not only the skeletal articulation, but the fascial articulations in the neck (deep, middle, superficial cervical fascia), the shoulder blade (endothoracic fascia), as well as the inter-muscular articulations.
Although it may be difficult to integrate "fascial articulations" into your mental hard drive, it should be easy to understand the obvious role of fascia in human movement...in both connection and disconnection. This provides a "bridge" to a more complete understanding of biomechanics...which is essentially the Trans-anatomical understanding of movement. Fascia is both friend and foe...when it is healthy and strong, you are feeling good. When it is damaged or otherwise unhealthy, it can be your worst enemy. From the most highly conditioned athlete to the the most severely affected child with Cerebral Palsy (who are near and dear to my heart), fascia is THE key fundamental structure in their health, maintenance, and development...period.
I hope the journey to date has been productive...and to those who are still "on the bus", part 3 will go into specifics about trans-anatomical movement and fascial articulations by using an age-old standard test (straight-leg lift) as an example. Hopefully it will engage and enlighten!
Cheers!
Saturday, October 1, 2011
Contextual Perspective on Orthotics, Splints, and Braces
The recent post by Leonid Blyum “Analytical Review: Cerebral Palsy and Forceful Devices-Orthoses, Splints, Braces” raised a number of fundamental important points regarding the use of “devices of external support”. One particular comment prompted some significant questions which then lead to some more evaluation and thought. Without going into detail about the actual thought process, I will simply get right to the point.
There seems to be a great deal of consensus regarding the benefits of the implementation of orthotics, braces, and splints. In fact, it is without question a “staple” protocol for almost every issue of mild to severe distortions of the feet. It goes without question that some form of AFO, KFO, lift, etc will be implemented as part of the rehabilitation plan. It isn’t my intention to debate “do they work or don’t they”…this question is far too simplistic and, quite honestly, a naïve way of approaching the topic. My intention is simply to take a step (or two) backwards and attempt to gain some perspective on the more fundamental question: “are these devices doing what I intend them to do?” To be precise, are they “fixing the feet”…are they preventing any further distortion…and are they creating a more “harmonious” environment for the user? These types of questions are either never asked or simply assumed to be yes, yes, and yes. Therefore, I would like to propose that the implementation of these devices be put into proper CONTEXT. By definition, my opinion as to their “therapeutic value” is completely dependent on the context they are being prescribed. The proper context is clearly explained in the video, therefore I won’t go into detail but I will expand on a very interesting analogy that was brought up that will offer some useful insight into what I have called “Contextual Perspective”.
Let us first consider a simple construct or continuum. Everything regarding biological systems can be classified as either “simple” or “complex”. For example, movement patterns can be considered simple or complex (in reality nothing is truly simple, but you get my idea). Let’s probe a little further and consider biological joints. You can argue that a hinge joint is a relatively simple joint…and a hip joint is relatively complex. You can also postulate that a single-jointed movement is simple and a multi-jointed movement is complex….there is an infinite amount of ways to organize this concept, but it should be relatively straight-forward.
If you accept this concept, then you must also accept that achieving biotensegral equilibrium in a simple joint is far simpler than achieving biotensegral equilibrium in a complex joint. If we look at an x-ray of a horses foot, we can easily see that the complexity of the horse’s “foot” (or hoof, to be precise) is relatively simpler than that of the human foot.
Although it is classified as “simple”, it most certainly is effective in performing it’s intended function.
If we move along this continuum a little more, we will move from the hoof to the more complex “paw”.
The paw (canine, feline for example) essentially contains the same general elements that the human hand and foot do, however it is organized in a very specific way which is clearly illustrated in the above image showing what could be considered metacarpals (purple bones) more or less fused together. However, there are more joints within it and therefore it’s organizational and proprioceptive demands are more involved. It can be assumed that the more complex paw can also perform more complex functions that are inherent in the feline and canine family (tigers, wolves, etc). These animals are extremely fast AND agile…the horse, although being fast, has a significantly poorer agility rating (if you have ever been around horses as much as I have, you will agree that horses trip a lot and are extremely uncomfortable on unstable and/or slippery footing).
Now we get to the human foot. When put into perspective, it is an absolute marvel of engineering. The human foot has 28 bones in it, therefore it has 84 separate potential planes of movement. This would most certainly deserve the classification of “complex”.
It’s complexity can be explained by evolution…we are biped and therefore have “two less points of contact with the ground”. Our horse, canine, and feline friends have the advantage of having four…therefore our 2 feet must be highly adaptable, sensitive, and capable of not only providing a stable platform , but allowing for multiple micro levels of movement that ultimately define our high level of agility.
What does all this mean and where does it fit into the issue of orthotics, splints, and braces??! If you’ve managed to get this far, then you are definitely worthy of some clarity! Given the obvious complexity of the human foot, it is somewhat naïve to assume that ANY adjustment at one SINGLE point of movement will produce any significant “improvement” in the condition of the foot. It is analogous to winning the lottery…yes, you may be extremely lucky and get the singular point of conflict that resolves all of your problems. However, the reality is that this is highly unlikely. Therefore my professional opinion as to the use of orthotics to “reduce distortion and improve the condition of the foot” currently remains highly skeptical at best. However, there is definitely a rationale for their use in improving comfort and reducing risk of further injury.
This statement can be explained as such: When braces are placed on the human foot, you essentially “block” the majority of the freedom within and “downgrade” the foot to a hoof. Obviously having a functional “hoof” is more productive than a distorted and painful foot. This is precisely what I mean by CONTEXTUAL PERSPECTIVE. It is also important not to stop there in this “contextual thinking”. The rest of the human body is designed with the idea that a “complex foot” is underneath…therefore, if we switch out a foot for a simpler “hoof”, there is a significant change in the force transmission to the knee and hip. Essentially, a significant amount of stress that was previously absorbed and distributed through the foot now bypasses it completely and impacts the knee and hip further up…keep this in mind when designing your treatment plan!!
This most certainly qualifies as a “rant”…so I will end with a very warm thank you for reading!!
Cheers.
Friday, September 30, 2011
Connective Tissue: Body-Wide Signaling Network?
Once again, i have caught the reading bug and have come across another intelligent article on the growing interest and study of connective tissue and it's implications in the human organism. I have found that the more you ask and the more you dig, you not only find answers but you uncover more questions! This particular article asks a very important and fundamental question: is connective tissue an immense signalling network? It was written 6 years ago and the more current research has shown this to be highly likely (if not true). It also makes another important point: the musculoskeletal system has been studied in relative isolation from the rest of the body...implying that connective tissue has no other function other than something mechanically based.
I am aware that not everyone has the time or energy to plow through scientific articles...it is an unlikely source of relaxation for me which most people do not share. Therefore, I have decided to insert the summary into my post because it very accurately captures the essense of the article. For those who are more curious...click the link and read on!
SUMMARY: Unspecialized ‘‘loose’’ connective tissue forms an anatomical network throughout the body. This paper
presents the hypothesis that, in addition, connective tissue functions as a body-wide mechanosensitive signaling
network. Three categories of signals are discussed: electrical, cellular and tissue remodeling, each potentially
responsive to mechanical forces over different time scales. It is proposed that these types of signals generate dynamic,
evolving patterns that interact with one another. Such connective tissue signaling would be affected by changes in
movement and posture, and may be altered in pathological conditions (e.g. local decreased mobility due to injury or
pain). Connective tissue thus may function as a previously unrecognized whole body communication system. Since
connective tissue is intimately associated with all other tissues (e.g. lung, intestine), connective tissue signaling may
coherently influence (and be influenced by) the normal or pathological function of a wide variety of organ systems.
Demonstrating the existence of a connective signaling network therefore may profoundly influence our understanding
of health and disease.
c 2006 Elsevier Ltd. All rights reserved.
Connective Tissue: BodyWide Signaling Network
Monday, September 26, 2011
“Analytical review. Cerebral Palsy and forceful devices- orthoses, splints, braces”
The link below will direct you to a very informative blog post from Leonid Blyum. The issue of splints, orthotics, braces, etc. when addressing the complex rehabilitation of children with Cerebral Palsy comes up with an alarming regularity. In my 6+ years of working directly with these special children and their families, it is undeniably one of the top 2 or 3 topics that always comes up. My main point is not that it SHOULDN'T be a topic of conversation, rather that it has become "standard operating procedure"...and that the use of these devices isn't even examined or questioned. To be more precise, the mere NOTION of asking "is this the best thing for my child and will it do what people are claiming it will do?" is sometimes beyond comprehension for alot of families. The reality is that these approaches have been in "mass circulation" for hundreds of years...the majority of the advancements being in the development of light, softer, and more durable implements...however there is still a fundamental question that remains: "What is the true biomechanical consequence of using these". There is far too much over-simplification when dealing with complex biomechanical disorders..."the foot is twisted in? Let's put on a hard brace to force it back" or "Oh, the hard brace hurts the foot? Ok, let's put a soft brace on". It would be ideal if it were that simple...and if it were, there certainly wouldn't be any need for therapeutic "experts". At any rate, the link to Leonid's post(with accompanying video) will prove to be extremely informative for ANY rehabilitation professional. The thought process and analytical approach extend beyond just cerebral palsy. It is in-depth and most certainly in my "must read" folder!
“Analytical review. Cerebral Palsy and forceful devices- orthoses, splints, braces”
Braces and orthoses in Cerebral Palsy ABR position Aug 2011 from BlyumABR on Vimeo.
Thursday, September 15, 2011
Redefining the Joint: Part 1
Why in the world would I suggest that the word "joint" be re-defined? It's a simple thing, right? Let's look at the definition as quoted in the Merriam-Webster Dictionary: the point of contact between elements of an animal skeleton with the parts that surround and support it . This definition conjures up the image that likely popped up in your mind...2 bones, some soft tissue around it, and maybe a meniscus in between.
The above image is nothing new to anyone. You have the pivot joint, the ball-and-socket joint, and the infamous hinge joint. This image follows the quoted definition quite nicely. The unfortunate thing is that the mechanics of human movement cannot be compacted into a simple definition and certainly not be explained by simple mathematical models. "Well, what is the right definition then?"...I would be naive to suggest that this definition is "wrong" per se, rather I merely suggest that it is very simplistic. Complex systems, by definition, demand complex explanation and understanding...therefore a more global perspective is required. As per "Gavin's New Trans-anatomical Dictionary", a joint is defined as: Linear and/or angular displacement between separate biological elements . To many of you, this may seem like a fancier way of saying the same thing...however, you couldn't be further from the truth. The reality is that the skeleton (bones) has a "monopoly" on everything joint-related. Why is this so?...by convention! It's in the dictionary, Gavin. But if you look at my definition, the skeleton is only a PART of it. Linear and/or angular displacement indeed occurs at all of the "typical" spots you would think of (knees, elbows, shoulders, etc)...however, if linear and/or angular displacement is a key element in this definition, you need to consider EVERY area that experiences this displacement as a true joint!!
It is not sufficient to suggest that movement only occurs at the "joints" and the soft tissue is simply a "biological sleeve" that fit over it. It clearly involves sliding of specific fascial layers one on top of the other. For example, the tendons of the wrist actively slide against each other when activated...which, by definition constitutes a joint. As you flex your arms, the fascial layers (from the skin to the triceps) on the back of the arm slide against each other and along the humerus...this constitutes a joint. The fundamental question is: who decides that if there is no bone, there is no joint?". If you consider the scenario where these movements are restrictied or blocked (fascial layers are "glued" together), you would have NO PRODUCTIVE MOVEMENT AT ALL. Therefore, when you consider this fact, the whole idea of "assessing range of motion" becomes something quite daunting...and perhaps even seemingly impossible. We therefore come to a crossroad of sorts. You can either go one way down "Newtonian Anatomical Model Boulevard" and be quite happy and comfortable with the status quo (which is a completely acceptable decision)...or you can go the other way and travel on "Trans-Anatomical Model Road" and walk a path of some unknowns and new discoveries.
I will go into more detail on the transanatomical definition of movement in part 2. For now, i will let you pause at the "crossroad"...digest the concept...and for all of you who choose Transanatomical Road, see you around the corner!
Wednesday, September 14, 2011
The Underlying "Diagnostic Disability".
I recently came to realize that there is an underlying problem within the health care system istelf that leads to more challenges for those seeking our "professional expert guidance". Like most of my "revelations", this came to me by chance through some recommended reading given to me by a collegue (gracias, Daiana!). This very insightful articles effectively describes that one of the main challenges to overcome is our inability to establish a "common language" among rehabilitation professionals. In effect, we are "diagnostically disabled". As explained in the article, the role as diagnostician for the physical therapist is quite challenging and is met with many dilemma's such as lack of consensus among professionals regarding classification, rapid evolution of new knowledge, and the complexity of the diagnostic process. I believe this is at the heart of a fundamental "dysfunctional attitude" among professionals. There is a constant sense of "competition for diagnosis" which inevitably leads to more confusion and frustration for the care-seeker. They are given different and sometimes conflicting information depending on who they refer to. The neurologist will make his / her comments...which may differ from the orthopedic surgeon...then when it comes to the physical therapist, he or she is commited to a plan of action that is contraindicated by the surgeon or even perhaps counter-intuitive to the care-seeker himself!
The article below is an excellent example of how self-examination and consistent search for solutions from within can result in significant positive impact, not only on a personal practice, but on the system as a whole. It also presents some constructive ideas on how to reduce the negative implications of this diagnostic disability on the care-seeker. It was a refreshing read and re-affirmed to me that constructive information can come from anywhere at any time...so keep your eyes peeled and, more importantly, your mind OPEN!.
Disabling Our Diagnostic Dilemmas
Monday, August 22, 2011
Spastic Muscles: Victim or Perpetrator?
This is perhaps one of the most counter-intuitive questions I have ever asked...and the answer is almost unanimously the same: "The muscles are the bad guys, therefore we need to attack them with an aggressive campaign of stretching...and if that doesn't work we always have botox". I'm exaggerating somewhat, however the only option families are given is overwhelmingly skewed to these drastic measures. As a professional (or as a parent / patient) it is fundamentally critical to examine all other options and not to simply "refer to my favorite textbook to see what the 'experts' say". The fundamental question is: "Are the muscles victims or perpetrators?" To be precise, are they THE problem or are they a SYMPTOM of a problem. In the overwhelming number of cases, muscle tension is SYMPTOMATIC (in both disorders of movement and posture AND the healthy population, by the way). Therefore, by definition the "treatment" protocol should be focused on the SOURCE of the problem. Unlike a common cold or flu, treating the symptoms leads to dead-ends and will result in future problems down the road.
In disorders of movement and posture like Cerebral Palsy, the muscular tension is a reflection of the profound compressional weakness that exists within the entire structure. For a better explanation of compressional weakness refer to my previous post, but in brief, compressional weakness is the absence of fundamental hydraulic strength which is responsible for support under the forces of gravity as well as the weight of the body itself. Essentially, when this vital component is missing, the muscles are asked to take on "double duty". They are actively solicited to compensate for the lack of compressional (passive postural) strength and therefore must be used to maintain balance...AND they are also called upon to perform the dynamic movement-based functions they are originally designed to do. It is no wonder that movement is so chaotic and uncontrolled...imagine using all of your muscles to maintain your balance AND perform movement at the same time.
Don't worry...I'm getting to the point. A strategic and focused protocol to improve compressional strength will subsequently result in a reduction in general muscular tension and rigidity. Period. Therefore my message is simple: STOP FIGHTING WITH THE VICTIMS! It is perhaps the most instinctive and inuitive thing to do, but history shows quite clearly that doing this is is a dead end street filled with false hope and "irresponsible dreaming".
Some of you may be saying "sounds good, but can it be done?" As the response to my previous post is showing...pictures are worth a thousand words. In that light, I have posted more amazing transformations that are an example of the potential to address muscle spasticity / rigidity at its true source. And remember...working with fascia is far from glamorous. It requires a significant amount of time and effort...but it is well worth it!
Cheers.
Analyzing the Source of Muscle Spasticity
Tuesday, August 16, 2011
The Role of Fascia in Cerebral Palsy...you can't miss this!
I have recently returned from Chile where I was working with another amazing group of children (and their families). It never ceases to amaze me how fortunate I am to be allowed the privilege to enter into their world and contribute to their child's progress. Each and every evaluation provides me with greater insight into the wonders of the human body...and for that I am eternally grateful. For those who have been curious enough to continue reading this blog, you are by now fully aware of my fascination for fascia and all that it implies. Although words (lots and lots of them)effectively convey this message, it is (more often than not) the actual pictures that demonstrate the full power and implication of this wonderful, and highly underrated, structure. I have performed many evaluations with children with disorders of movement and posture over the years...and there is a common thread that binds almost all of their families together: "Gavin, I just want a better life for my child. I want him/her to be happy and healthy and ultimately give them the absolute most that can be given to help them". Something as simple as being able to sit independantly can seem trivial to us, but can mean the world for these special children and special families. Therefore, I put it to anyone who questions the implications that fascia has on movement and posture...look at this example and formulate an intelligent, articulate, and logical reason not to admit the enormous opportunity and potential for improvement that exists. Although I have a plethora of examples, the one I have posted is the freshest in my mind and is also without possibility of mis-interpretation. One year of specific focus and hard work can bring about life-changing results! I hope it inspires you, fascinates you, and most importantly...stimulates some constructive curiosity!
Fascial Strengthening in Cerebral Palsy
Thursday, August 4, 2011
Coming Soon: Fascia and Fibromyalgia
I am very excited about this upcoming post because it will be the first look into some innovative techniques using the extended fascial paradigm in the treatment of a specific pathology. I recently stumbled upon an interesting article that outlines the role that fascia plays in Fibromyalgia. More importantly, how it may be a potential source of both the "problem" and the "solution" simultaneously. It is well known that massage has been a largely effective treatment for the reduction of symptomatic pain associated with fibromyalgia. Whereas some believe that the common "villain" is the muscle, there is growing evidence that fascial dysfunction is a more likely culprit. Therefore, any improvements to the delivery, absorption, and effective range of massage will help in relieving discomfort and pain. I will be outlining the Soft Ball Massage Technique in my next post, however I think it would be helpful to have a look at the article itself and get a fundamental look at the rationale behind this proposed technique. Enjoy and stay tuned for Soft Ball Rolling Massage!
Fibromyalgia and the Fascia Effect
Monday, August 1, 2011
Myth, Madness, or New Frontier?
Once again...another posting of an article on fascia. To be honest, it has been difficult to hold back on posting all of the wealth of existing study, research, and scientific evidence of the significance of fascia and connective tissue. I promise more original material, however I think my recent postings of Myers, Van der Wal, and Schleip will greatly enhance the general understanding that this is no myth...this fascia "stuff" is important! So it begs the question: is this myth, madness, or a new frontier? Some would agree that connective tissue is a simple "shrink wrap" for the muscles and just basically holds things in place and therefore considering it as an "active player" in musculoskeletal dynamics is pure MADNESS. Others, in their infinite ignorant wisdom, would tell you that it's purely MYTH..."studies are pure speculation and inconclusive". The reality is that connective tissue is not only the focus of increased in research protocols, but is proving to be quite relevant in the human organism. The potential implications give it the well deserved title of NEW FRONTIER. This was one of the first articles I read regarding fascial properties and it stuck with me throughout my formulations and developing understanding of the role of connective tissue and fascia. Paste it into your mental hardrive. Cheers.
Active Fascial Contractility
Subscribe to:
Comments (Atom)