Saturday, October 22, 2011
Pediatric Evaluation 101
I typically avoid back-to-back posts...prefering to let a post "marinate" in the minds of the reader for at least a week. However, I have recently been actively involved with my work with children with Cerebral Palsy (ABR) and it has only recently occured to me that alot of our evaluation protocol is still somewhat foreign to the many parents and family members. The purpose has become so integrated in my mind, that I haven't truly considered that anyone wouldn't understand, not only WHAT I'm doing, but WHY I'm doing it. In essense, I have overlooked an essential element of any successful assessment: UNDERSTANDING BY THE PARENT / CARE-SEEKER.
With this in mind, I have decided to post a series of "back to school" postings designed specifically to EDUCATE parents on the essentials of typical pediatric assessment protocols. It is my firm belief that, with understanding, you will become more involved in the process of your child's development. In this spirit, I have used a photo of Concordia University in Montreal at the beginning of this post. Not only did I receive my Bachelor of Science degree there, but I went on to teach as a laboratory instructor for 5 fun-filled years. So....class, attention please:
The first "class" is simply to familiarize you with a few basic tests and give you some insight into its purpose. Before I continue, I will remind you of an important point I raised in a posting from June (Trainers Corner: Back to Basics): Consider your child's developmental age in light of the chronological age. In children with disorders of movement and posture, improvement is gauged by the progressive movement through developmental milestones. Therefore, the normal developmental process is your guide. The following are some select tests, with their respective rationale and corresponding developmental stages:
The Prone Position: In the prone position, the baby is now able to bring his head up and look forward with the head being 45 to 90 degrees off the mat. Weight is borne on the forearms. When the head and chest are well off the mat, the baby is ready to start to roll from the prone to the supine position. Rolling front to back usually occurs at 3 to 5 months of age. Rolling over too early can be due to excessive extensor tone. In essense, any functional performance that includes rolling or propping on the hands is dependant on this prior stage.
The Landau Reflex: The Landau is an important postural reflex and should develop by 4 to 5 months of age. When the infant is suspended by the examiner’s hand in the prone position, the head will extend above the plane of the trunk. The trunk is straight and the legs are extended so the baby is opposing gravity. When the examiner pushes the head into flexion, the legs drop into flexion. When the head is released, the head and legs will return to the extended position. The development of postural reflexes is essential for independent sitting and walking. This particular test is not typically done, but can be valuable when more comprehensive discussion on sitting and walking become realistic.
Lateral Propping: Lateral propping or protective extension is essential for the baby to be able to sit independently. This postural reflex develops at 5 to 7 months of age. Anterior propping actually develops first, then lateral propping. For anterior propping the baby will extend the arms forward to catch himself and prevent falling forward. Lateral propping occurs when the baby is falling to one side or the other and he extends the arm laterally to catch himself. Asymmetric lateral propping can be an early sign of hemiparesis. The baby will prop on one side but on the paretic side he will not extend the arm to catch himself.
The Parachute Test (Flying Test): The parachute reflex is the last of the postural reflexes to develop. It usually appears at 8 to 9 months of age. When the baby is turned face down towards the mat, the arms will extend as if the baby is trying to catch himself. Prior to developing this reflex, the baby will actually bring the arms back to the plane of the body and away from the mat.
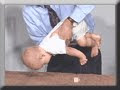
Traction Test: On traction, which is pulling to a sitting position, the baby has good head and trunk control. The head and shoulders are flexed forward and the arms are flexed. The baby actively helps himself to get to the sitting position by pulling with the arms. Also notice that the legs are flexed at the hips and are off the mat as the baby pulls himself to sitting. On being laid back down to the supine position, the baby doesn’t flop back, but is able to control the lowering of his head and trunk to the mat. This particular test should be very familiar to the ABR readers. How is "good head control" assessed? More importantly, what are the bare essentials needed to have minimal head control? The traction test is a valuable tool that gives excellent feedback and lends towards a more efficient treatment protocol.
In North America, coffee is just as important to the learning process as is a laptop...so, grab a cup of "Joe" (for my South American friends, un cafe con leche) and get to work.
Class dismissed.
Cheers! =)
Subscribe to:
Post Comments (Atom)






Very interesting stuff, Gavin. In a therapy which I use to prep Adam's body for ABR, I've learned that brain injury can result in the defensive re-establishment of a lot of these primitive reflexes which should have been extinguished and integrated in the womb or the first six months. In brain injury, CP, etc., these reflexes persevere and hinder development. We use a cold laser to help integrate stuff like the startle reflex so Adam can better receive ABR. Interesting.....
ReplyDeleteIndeed! What I am discovering is the presence of these primitive reflexes in kids that are into 4,6,8 years of age...when they should have been extinguished (as you say) by the first 4-6 months. The Landau, Moro, and Gallant Reflex...very interesting indeed. I'm curious about the cold laser, though. I'll have to look into that!
ReplyDeleteIf interested, Gavin, here's a link to the program I use:
ReplyDeletehttp://www.reflexintegration.net/
Interested! Thanks, Phil!
ReplyDeleteGav recorde a mi profesora de pediatria y psicomotricidad reconozco q desde la mirada de ABR es aún mas interesante eres un gran maestro
ReplyDeleteNancy